Description: Your Comprehensive Guide to Respiratory Wellness in Modern India
Welcome to the most detailed and practical guide on protecting your lung in the challenging environmental conditions of 2026 India. This comprehensive resource has been carefully crafted to address the growing respiratory health crisis affecting millions of Indians across every age group and socioeconomic background. The air we breathe today contains pollutants and particles that our grandparents never encountered, and our bodies are struggling to adapt to this new reality. Medical experts from India’s premier institutions including AIIMS Delhi, Medanta Hospital, and Manipal Hospitals have contributed their knowledge and insights to create this essential guide that bridges the gap between complex medical science and practical daily application. Within these pages, you will discover ten powerful strategies that work together to create a complete respiratory protection system tailored specifically for Indian living conditions. Each strategy has been explained in detail with clear, actionable steps that anyone can follow regardless of their background or resources. You will learn how to transform your home into a clean air sanctuary, how to use the incredible power of Indian superfoods to strengthen your lungs from within, and how ancient breathing techniques can dramatically improve your lung capacity and resilience. The guide addresses the silent epidemic of undetected lung disease that affects nearly 95 percent of COPD cases in India, showing you exactly how to recognize early warning signs and when to seek professional help. You will understand why winter months pose special dangers and how to adjust your daily routine to stay safe when temperatures drop and pollution peaks. The critical importance of exercise appears throughout this guide, but with the essential caveat that when and where you exercise matters as much as whether you exercise at all. Traditional Indian remedies receive the scientific validation they deserve, with explanations of how tulsi, amla, haldi, and other kitchen staples actually work at the cellular level to protect respiratory tissues. Tobacco cessation receives comprehensive treatment because eliminating this single risk factor does more for lung health than any combination of other interventions possibly could. Finally, you will learn how to build a lifelong respiratory health system that evolves with you as you age and as environmental conditions change. This guide represents thousands of hours of research synthesis and practical experience, all distilled into language that remains accessible while never sacrificing scientific accuracy. Whether you are a concerned parent in Delhi-NCR, a young professional in Bengaluru breathing traffic fumes daily, a homemaker in Kerala spending hours in the kitchen, or a student worried about how pollution affects your studies and sports performance, this guide has been written specifically for you. The knowledge contained here has the power to add years to your life and life to your years by preserving the precious gift of healthy breathing. We invite you to read carefully, take notes, share with family members, and most importantly, take action starting today because your lungs cannot wait for policy changes or technological miracles that may never arrive.
1: Understanding the Complex Landscape of Lung Health Crisis in 2026 India
The Critical Importance of Comprehensive Lung Health Protection Strategies
The human respiratory system represents one of the most sophisticated and delicate mechanisms in the entire body, processing approximately 11,000 litres of air daily while filtering out countless harmful particles and pathogens. In the context of modern India, this remarkable system faces unprecedented challenges that demand our immediate attention and action. Leading medical institutions including Medanta Hospital have launched extensive year-round respiratory health initiatives because they recognize a fundamental shift in how environmental factors affect human health . The traditional understanding that air pollution only harms us during winter months has been completely overturned by scientific evidence showing year-round danger across the entire Indo-Gangetic plain and major metropolitan areas. This reality makes the adoption of robust lung health protection strategies not merely advisable but absolutely essential for every individual regardless of age or location. The particulate matter penetrating our respiratory systems consists of microscopic particles measuring less than 2.5 micrometres, small enough to bypass our natural defences and enter deep lung tissue where they trigger inflammatory responses and cellular damage that accumulates over time.
Advanced Understanding of Environmental Threats Requiring Lung Health Protection Strategies
The nature of respiratory threats in 2026 has evolved far beyond visible smoke or industrial emissions. Contemporary urban environments expose residents to complex mixtures of vehicular exhaust, construction dust, secondary organic aerosols formed through atmospheric chemical reactions, and even microplastic particles suspended in the air. Dr. Naresh Trehan’s warning about modern lifestyles “silently stealing years from our lives” carries profound weight when we examine the epidemiological data . Research published in leading medical journals demonstrates that chronic exposure to elevated pollution levels reduces life expectancy across India by an average of 3.5 years, with residents of Delhi facing reductions of up to 8.2 years. This damage accumulates insidiously through mechanisms including oxidative stress that damages cellular DNA, chronic inflammation that remodels airway architecture, and epigenetic changes that may predispose future generations to respiratory illness. Understanding these mechanisms allows us to appreciate why superficial solutions prove inadequate and why comprehensive lung health protection strategies must address multiple pathways of injury simultaneously.
Practical Implementation of Advanced Lung Health Protection Strategies
Moving from theoretical understanding to practical action requires systematic engagement with environmental monitoring and personal behaviour modification. Begin by downloading and regularly consulting multiple AQI applications including SAFAR which provides data from over 200 monitoring stations across India, and AirVisual which offers global comparative data that helps contextualize local readings. Establish the discipline of checking these readings every morning before planning outdoor activities, treating AQI above 200 as a red alert requiring modified behaviour. Educate yourself about the specific pollutants prevalent in your region, whether PM2.5 from vehicular sources, PM10 from construction, or ozone formed through photochemical reactions during summer months. Share this knowledge systematically with family members, particularly older relatives who may dismiss respiratory symptoms as inevitable accompaniments of aging. Document your own respiratory symptoms over time, noting correlations with pollution spikes, weather changes, or seasonal factors. This personal data proves invaluable when consulting healthcare providers and allows you to refine your lung health protection strategies based on individual response patterns rather than generic advice alone.
2: Comprehensive Approaches to Early Detection of Respiratory Diseases
The Critical Role of Screening in Modern Lung Health Protection Strategies
The epidemiological landscape of respiratory disease in India presents a troubling paradox wherein the majority of affected individuals remain completely unaware of their condition until irreversible damage has occurred. Medical researchers estimate that between 95 and 98 percent of chronic obstructive pulmonary disease cases across India escape clinical detection, while approximately 70 percent of severe asthma sufferers continue without proper diagnosis or treatment . This detection gap represents not merely a statistical curiosity but a human tragedy of immense proportions, as individuals live with progressive breathlessness, declining functional capacity, and mounting disability while attributing their symptoms to normal aging or temporary indisposition. Dr. Randeep Guleria’s observation that lung damage accumulates silently before announcing itself through unmistakable symptoms highlights the fundamental challenge facing respiratory medicine . The cough that seems insignificant, the mild breathlessness during stair climbing, the fatigue that appears disproportionate to exertion, all represent potential early warnings that too often go unheeded until emergency intervention becomes necessary.
Scientific Basis for Proactive Detection as Lung Health Protection Strategies
Understanding why lung diseases escape detection requires appreciation of respiratory physiology and the remarkable reserve capacity built into human lungs. Most individuals possess approximately 30 to 50 percent more lung capacity than required for daily activities, meaning significant tissue destruction can occur before symptoms manifest during ordinary routines. This physiological reserve, while evolutionarily advantageous, becomes problematic when it masks progressive disease until functional impairment reaches advanced stages. Additionally, the human capacity for adaptation means individuals unconsciously reduce activity levels to accommodate declining respiratory function, interpreting their decreasing engagement with physically demanding activities as natural consequences of aging rather than pathological processes requiring medical attention. The insidious nature of this adaptation explains why so many patients first seek medical attention when already experiencing significant disability. Effective lung health protection strategies must therefore circumvent these natural compensatory mechanisms by establishing objective measurements of respiratory function that reveal changes before they become subjectively apparent.
Systematic Approaches to Implementing Advanced Lung Health Protection Strategies
Establishing effective respiratory surveillance requires moving beyond symptom-based healthcare to proactive screening protocols integrated into routine health maintenance. Begin by understanding that any cough persisting beyond three weeks warrants professional evaluation regardless of apparent severity or associated symptoms. Schedule an appointment with a physician specifically to discuss respiratory health, bringing documentation of any breathing difficulties, cough patterns, or activity limitations you have observed. Request spirometry testing specifically, understanding that this simple procedure requiring only that you exhale forcefully into a calibrated instrument provides objective data about airway function that physical examination alone cannot reveal. For individuals residing in high-pollution urban environments, annual spirometry should become as routine as blood pressure measurement or cholesterol screening. If you have family history of respiratory disease, whether asthma, COPD, or lung cancer, maintain heightened vigilance and consider more frequent evaluation. Recognize that early-stage respiratory disease often responds dramatically to appropriate intervention, while advanced disease requires complex management with more limited outcomes. These lung health protection strategies transform your relationship with respiratory health from reactive crisis management to proactive wellness maintenance.
3: Advanced Indoor Environmental Management for Respiratory Protection

Creating Therapeutic Indoor Environments Through Lung Health Protection Strategies
The assumption that retreating indoors provides automatic protection from outdoor air pollution represents one of the most dangerous misconceptions in contemporary environmental health. Scientific measurements consistently demonstrate that indoor air quality frequently equals or even exceeds outdoor pollution levels, particularly in Indian homes where multiple indoor sources combine with inadequate ventilation and outdoor infiltration . The concentration of harmful particulate matter inside homes during cooking hours can reach levels ten to twenty times higher than simultaneous outdoor measurements, exposing family members to extreme respiratory challenges during daily activities they consider completely safe. Children who spend most of their time indoors, elderly relatives who rarely venture outside, and homemakers who work for hours in kitchen environments face cumulative exposures that may exceed those experienced by outdoor workers. This reality fundamentally reorients our understanding of lung health protection strategies, requiring that we apply the same rigorous attention to indoor environments that we traditionally reserve for outdoor air quality monitoring.
Scientific Principles of Indoor Air Purification as Lung Health Protection Strategies
Effective indoor air management rests on understanding the physics and chemistry of airborne particles and their behaviour within enclosed spaces. Particulate matter of various sizes exhibits different settling characteristics, with larger particles settling relatively quickly while fine PM2.5 particles remain suspended for hours or days, continuously available for inhalation. Gaseous pollutants including nitrogen dioxide from gas cooking, volatile organic compounds from furnishings and cleaning products, and ozone from electronic equipment create additional respiratory challenges requiring different mitigation approaches. HEPA filtration technology, when properly implemented with adequate clean air delivery rates matched to room size, can remove up to 99.97 percent of airborne particles down to 0.3 micrometres, providing substantial protection when units operate continuously. Dr. Ritu Singh’s emphatic recommendation to prioritize HEPA filter investment reflects hard economic reality, these devices represent capital expenditure protecting irreplaceable biological assets. The eight to ten hours of clean air provided during sleep allow respiratory tissues to recover from daytime exposures, potentially breaking the cycle of continuous inflammation that characterizes chronic respiratory disease progression.
Comprehensive Indoor Management Implementing Lung Health Protection Strategies
Transform your living space through systematic interventions addressing all significant pollution sources. Begin with HEPA filtration in bedrooms and main living areas, selecting units with clean air delivery rates appropriate for room dimensions and operating them continuously on low settings rather than intermittently on high. Replace traditional dry sweeping with wet mopping using microfiber materials that capture rather than redistribute dust, and consider investing in vacuum cleaners equipped with HEPA filtration to prevent exhaust plumes from recirculating collected particles. Reconsider traditional practices including agarbatti burning, dhoop lighting, and mosquito coil use, which generate substantial particulate matter within enclosed spaces, seeking alternatives such as essential oil diffusers for fragrance and physical barriers for insect control. Upgrade kitchen ventilation through chimney installation with adequate capture efficiency and exterior exhaust, and develop habits of using range hoods during all cooking activities regardless of apparent smoke production. Integrate humidity management through humidifier use during dry winter months when respiratory mucosa become vulnerable, and dehumidifier operation during monsoon conditions when mould growth threatens respiratory health. These comprehensive lung health protection strategies transform homes from passive shelters into active respiratory health promoters.
4: Nutritional Biochemistry and Respiratory Defence Mechanisms
Dietary Modulation of Pulmonary Health Through Lung Health Protection Strategies
The intimate connection between nutrition and respiratory function operates through biochemical pathways that modern science increasingly understands and ancient traditions long recognized. Every breath of polluted air initiates oxidative cascades within lung tissues, generating reactive oxygen species that damage cellular membranes, modify proteins, and induce mutations in DNA that may ultimately trigger malignant transformation. The body’s endogenous antioxidant systems, including glutathione, superoxide dismutase, and catalase, work continuously to neutralize this oxidative burden, but their capacity can be overwhelmed by sustained environmental assault. Dietary antioxidants serve as essential reinforcements for these endogenous systems, providing the molecular tools necessary to maintain redox balance within respiratory tissues. This understanding elevates nutritional choices from matters of general wellness to specific lung health protection strategies with measurable impacts on respiratory disease risk and progression. The traditional Indian kitchen, with its emphasis on spices, herbs, and seasonal produce, contains precisely the compounds modern nutritional science identifies as most valuable for pulmonary protection.
Advanced Understanding of Protective Nutrients as Lung Health Protection Strategies
The mechanisms through specific nutrients protect respiratory tissues reveal the sophistication of evolutionary adaptations to environmental challenges. Vitamin C, concentrated in amla at levels exceeding most other natural sources, functions as a primary aqueous-phase antioxidant that directly neutralizes reactive species before they damage cellular components while also regenerating oxidized vitamin E, extending its protective effects. Curcumin from turmeric modulates inflammatory signalling pathways at the molecular level, inhibiting NF-kB activation that drives pro-inflammatory gene expression and reducing the chronic inflammation characterizing pollution-exposed lungs. Gingerols and shogaols from fresh ginger demonstrate bronchodilatory effects comparable to some pharmaceutical agents while also suppressing mucus hypersecretion that obstructs airways. Quercetin from onions and apples stabilizes mast cells, preventing inappropriate release of inflammatory mediators that trigger asthma attacks. Omega-3 fatty acids from fish and flaxseed incorporate into cell membranes, altering their physical properties and signalling characteristics in ways that reduce inflammatory responsiveness. Understanding these mechanisms allows intelligent selection of lung health protection strategies targeting specific vulnerabilities based on individual exposure patterns and health status.
Practical Integration of Protective Nutrition into Daily Life
Transform theoretical nutritional knowledge into daily practice through systematic incorporation of protective foods into established meal patterns. Begin each day with fresh amla, whether as juice, murabba, or simply sliced fruit, establishing baseline antioxidant protection before environmental exposures accumulate. Prepare turmeric milk using actual turmeric root rather than powder when possible, adding black pepper to enhance curcumin absorption by approximately 2000 percent through piperine-mediated inhibition of hepatic glucuronidation. Incorporate garlic and ginger into cooking not merely for flavour but as deliberate therapeutic additions, allowing their compounds to infuse into prepared dishes. Maintain regular consumption of seasonal fruits, understanding that vitamin C content varies dramatically between fresh and stored produce, making locally sourced options nutritionally superior. Prepare traditional kadha during pollution spikes or illness episodes, combining tulsi, mulethi, black pepper, and other respiratory herbs in decoctions that deliver concentrated phytochemicals to respiratory tissues. Maintain optimal hydration through warm water consumption throughout the day, understanding that adequate hydration maintains mucus rheology appropriate for effective mucociliary clearance. These nutritional lung health protection strategies create internal environments resistant to pollution-induced damage while supporting repair processes when exposures occur.
5: Advanced Respiratory Physiotherapy and Breathing Mechanics
Optimizing Ventilatory Function Through Lung Health Protection Strategies
The mechanical aspects of breathing receive insufficient attention in conventional discussions of respiratory health, yet they fundamentally determine how effectively lungs perform their essential functions. Most individuals, particularly those engaged in sedentary occupations, develop breathing patterns characterized by shallow thoracic excursions, accessory muscle overuse, and inefficient gas exchange that progressively weakens respiratory musculature while compromising ventilation of dependent lung regions. This mechanical inefficiency creates vicious cycles wherein inadequate ventilation leads to atelectasis and secretion retention, which further impair ventilation and create environments conducive to bacterial colonization. The diaphragm, designed as the primary muscle of inspiration, becomes weak and atrophic while neck and shoulder muscles recruited as substitutes fatigue easily and cannot sustain adequate ventilation during increased demand. Correcting these mechanical inefficiencies through targeted interventions represents some of the most cost-effective lung health protection strategies available, requiring no equipment beyond conscious attention and yielding benefits extending far beyond respiratory function to include stress reduction and autonomic nervous system regulation.
Scientific Basis for Breathing Retraining as Lung Health Protection Strategies
Understanding the physiology of optimal breathing illuminates why specific techniques prove beneficial and how they should be applied. Diaphragmatic breathing, the foundation of respiratory retraining, recruits the primary inspiratory muscle in coordinated contraction that draws air into lung bases where perfusion is greatest, optimizing ventilation-perfusion matching and gas exchange efficiency. The negative intrathoracic pressure generated during diaphragmatic inspiration also promotes venous return to the heart, enhancing cardiac output and systemic oxygen delivery. Pursed-lip breathing, intuitively adopted by many individuals with obstructive lung disease, generates back-pressure within airways that prevents premature airway collapse during exhalation, allowing more complete lung emptying before the next breath. This technique proves particularly valuable during exercise or stress when breathing rate increases and expiratory time shortens. Slow, deep breathing at approximately six breaths per minute, the rate historically associated with yogic practices, entrains cardiovascular rhythms through respiratory sinus arrhythmia, enhancing heart rate variability and vagal tone in ways that reduce sympathetic activation and stress hormone release. These physiological effects transform simple breathing exercises into powerful lung health protection strategies with measurable impacts on multiple organ systems.
Systematic Implementation of Breathing Optimization Techniques
Develop a comprehensive breathing practice through progressive mastery of foundational techniques before advancing to integrated applications. Begin with diaphragmatic breathing practice in supine position, placing one hand on chest and another on abdomen to provide sensory feedback confirming appropriate movement patterns. Inhale slowly through nose, allowing abdomen to rise while chest remains relatively still, then exhale passively through nose or pursed lips, feeling abdomen fall. Practice for five to ten minutes daily, gradually extending duration as technique improves and transferring practice to seated and standing positions. Add pursed-lip breathing during activities causing breathlessness or during scheduled practice sessions, maintaining awareness of exhalation control. Progress to pranayama techniques including Anulom Vilom (alternate nostril breathing), which balances autonomic nervous system activity while clearing nasal passages, and Bhramari (humming bee breath), whose vibratory effects stimulate parasympathetic pathways and may enhance nitric oxide production within paranasal sinuses. Integrate breathing awareness throughout daily activities, noting how stress, posture, and environmental factors affect breathing patterns, and applying learned techniques to normalize ventilation during challenges. These advanced lung health protection strategies build respiratory reserve while providing tools for immediate symptom management when needed.
6: Seasonal Adaptation and Environmental Rhythm Management

Circannual Rhythms in Respiratory Health Requiring Lung Health Protection Strategies
The human respiratory system evolved within environments characterized by predictable seasonal variations, developing physiological adaptations that optimize function across changing conditions. Modern urban environments, particularly in regions like North India, disrupt these evolutionary expectations through extreme seasonal contrasts combined with anthropogenic pollution that varies independently of natural cycles. The winter months bring cold, dense air that traps pollutants near ground level while simultaneously inducing bronchoconstriction through direct airway cooling and drying. Summer introduces different challenges including photochemical smog formation driven by intense sunlight acting on precursor pollutants, creating ozone concentrations that irritate airways and trigger inflammatory responses. Monsoon conditions foster fungal and mould growth while increasing humidity that can precipitate asthma symptoms in susceptible individuals. Effective lung health protection strategies must therefore incorporate seasonal awareness, adjusting behaviours and interventions to match prevailing conditions rather than applying identical approaches throughout the year.
Clinical Observations Guiding Seasonal Lung Health Protection Strategies
Medical researchers at AIIMS Delhi have documented patterns of respiratory morbidity that clearly reflect seasonal influences, with emergency department visits for respiratory complaints peaking during cold waves when temperature inversions trap pollution near ground level and cold air directly challenges airway reactivity . These observations carry practical implications for behaviour modification, suggesting that activity timing, exercise intensity, and protective measures should vary systematically with seasonal conditions rather than following rigid daily routines. The physiological stress imposed by breathing cold, polluted air combines thermal and chemical challenges that may synergistically exceed the effects of either factor alone. Cold air inhalation triggers reflex bronchoconstriction through direct airway cooling and activation of irritant receptors, while simultaneously reducing mucociliary clearance efficiency through impaired ciliary function. When polluted air provides the chemical irritants inhaled during this vulnerable state, the combined insult may overwhelm respiratory defences that might adequately handle either challenge separately. Understanding these interactions allows refinement of lung health protection strategies to address season-specific vulnerabilities.
Practical Seasonal Adaptation Through Targeted Lung Health Protection Strategies
Develop a seasonal calendar organizing respiratory protection activities around predictable environmental changes affecting your region. During winter months, reschedule outdoor exercise to late morning or early afternoon when temperatures have moderated and surface heating promotes vertical air mixing that disperses accumulated pollutants. Implement enhanced face covering protocols using N95 masks or multiple-layer scarves that warm and humidify inspired air while filtering particulate matter. Monitor indoor humidity levels, using humidifiers to maintain optimal moisture when heating systems dry indoor air to levels irritating respiratory mucosa. During summer, remain aware that clear skies and good visibility do not guarantee healthy air, as ozone formation peaks during afternoon hours when sunlight intensity maximizes photochemical reactions. Schedule outdoor activities for morning hours before ozone accumulation reaches peak levels. During monsoon, address indoor mould through improved ventilation, dehumidifier use, and prompt remediation of water intrusion or condensation sites. Throughout all seasons, maintain heightened vigilance during transition periods when rapid weather changes stress adaptive capacity and when pollution episodes may coincide with temperature extremes. These temporally sensitive lung health protection strategies optimize protection while minimizing unnecessary restrictions on quality of life.
7: Exercise Physiology and Pulmonary Rehabilitation Principles
Mechanisms of Exercise-Mediated Lung Protection Through Lung Health Protection Strategies
Physical activity induces physiological adaptations that extend far beyond cardiovascular conditioning, fundamentally reshaping respiratory structure and function in ways that enhance resilience against environmental challenges. Regular aerobic exercise stimulates angiogenesis within pulmonary capillaries, increasing the vascular surface area available for gas exchange and reducing the diffusion distance oxygen must traverse from alveoli to red blood cells. Ventilatory muscles, including the diaphragm, intercostals, and accessory muscles, undergo strength and endurance training that increases maximal voluntary ventilation and delays fatigue during sustained activity. Mucus clearance mechanisms improve through increased airflow velocities and the mechanical agitation accompanying whole-body movement, reducing secretion retention that otherwise impairs ventilation and harbours pathogens. Perhaps most significantly, exercise induces hormetic responses, mild stress that triggers cellular adaptations enhancing resistance to more severe subsequent challenges, including upregulation of antioxidant enzymes and heat shock proteins that protect against pollution-induced oxidative damage. These adaptations establish regular physical activity as fundamental among lung health protection strategies, providing benefits no pharmacological intervention can replicate.
Advanced Exercise Prescription for Respiratory Optimization
Designing exercise programmes for respiratory health requires consideration of intensity, duration, frequency, and environmental conditions that determine both immediate safety and long-term adaptation. Moderate-intensity aerobic activity, defined as exercise during which conversation remains possible but singing would prove difficult, provides optimal stimulus for respiratory adaptation while remaining sustainable for most individuals. Target duration of at least 150 minutes weekly, distributed across most days, to accumulate sufficient training stimulus for physiological adaptation. Include interval training elements periodically, alternating higher-intensity efforts with recovery periods, to challenge maximal ventilatory capacity and prepare respiratory systems for unpredictable demands. Incorporate resistance training addressing upper body musculature, as chest and shoulder strength supports optimal breathing mechanics and posture facilitating full lung expansion. Swimming deserves special consideration as optimal exercise for respiratory health, combining controlled breathing requirements that enhance ventilatory control with humidified air that minimizes airway drying and irritation. The warm, moist environment of indoor pools proves particularly beneficial for individuals with reactive airways who experience bronchoconstriction during land-based exercise in cold or dry conditions. These exercise-based lung health protection strategies build physiological reserve while providing immediate symptomatic benefits.
Environmental Intelligence Guiding Exercise Implementation
The benefits of exercise must be balanced against risks of increased pollutant exposure during outdoor activity, requiring sophisticated decision-making about when and where to exercise. Before each session, consult real-time AQI data from reliable sources, understanding that moderate exercise in moderately polluted air may produce net benefit while vigorous exercise in heavily polluted air may cause net harm. When AQI exceeds 150, consider indoor alternatives including home exercise equipment, gym facilities with adequate filtration, or mall walking in climate-controlled environments. When outdoor exercise proves necessary or preferable, select routes minimizing traffic exposure by choosing parks, residential streets, or green spaces away from major roadways. Time exercise to avoid peak pollution periods, generally early morning and evening during winter when inversions trap emissions, and afternoon during summer when ozone peaks. Monitor individual symptoms during and after exercise, noting any cough, wheeze, or unusual breathlessness that might indicate excessive exposure or exercise-induced bronchoconstriction requiring medical evaluation. Maintain heightened awareness during wildfire events, crop burning seasons, or industrial incidents when pollution may reach extreme levels unsafe for any outdoor activity. These intelligent lung health protection strategies maximize exercise benefits while minimizing environmental risks.
8: Integrative Approaches Combining Traditional and Modern Medicine
Synergistic Benefits of Combined Therapeutic Traditions as Lung Health Protection Strategies
The dichotomy often drawn between traditional and modern medicine represents a false choice that deprives patients of valuable therapeutic options from both systems. Contemporary medical science increasingly validates mechanisms underlying traditional practices while traditional systems offer holistic approaches addressing aspects of health that reductionist biomedical models may neglect. Ayurveda’s understanding of respiratory health, organized around Kapha dosha concepts and emphasizing preventive practices, provides frameworks for daily and seasonal routines that complement modern pharmacological interventions. The rasayana (rejuvenation) therapies targeting respiratory tissues through specific herbal formulations and detoxification procedures offer potential for tissue repair and resilience enhancement beyond what conventional medicine currently provides. Conversely, modern diagnostic capabilities including spirometry, imaging, and biomarker analysis identify specific pathologies requiring intervention while monitoring treatment response with precision impossible in pre-scientific eras. Intelligent integration of these complementary approaches creates lung health protection strategies more comprehensive and effective than either tradition alone could provide.
Scientific Validation of Traditional Respiratory Therapies
Research methodologies increasingly capable of investigating complex botanical preparations validate many traditional practices while identifying specific mechanisms accounting for observed benefits. Tulsi (Ocimum sanctum) demonstrates adaptogenic properties that normalize physiological responses to stress while exhibiting direct antimicrobial activity against respiratory pathogens and immunomodulatory effects enhancing host defence. Mulethi (Glycyrrhiza glabra) contains glycyrrhizin with demonstrated anti-inflammatory and expectorant properties, while also exhibiting antiviral activity against multiple respiratory viruses through inhibition of viral replication. Pippali (Piper longum) enhances bioavailability of other therapeutic compounds while demonstrating direct bronchodilatory effects through smooth muscle relaxation. The traditional practice of Jal Neti, nasal irrigation with warm saline, receives support from clinical trials demonstrating reduced symptom days and medication use in chronic sinusitis and allergic rhinitis, with effects mediated through mechanical clearance of inflammatory mediators and improved mucociliary function. Steam inhalation with aromatic compounds, when performed correctly, provides symptomatic relief through airway hydration, mucus liquefaction, and possible direct antimicrobial effects of volatile compounds. Understanding this scientific basis allows confident integration of traditional practices into comprehensive lung health protection strategies.
Practical Integration Creating Personalized Respiratory Care
Develop personalized respiratory care protocols drawing appropriately from both medical systems based on individual circumstances, preferences, and responses. Establish baseline respiratory function through modern diagnostic assessment, documenting any abnormalities requiring monitoring or intervention. Implement daily preventive practices drawn from traditional systems, including appropriate oil application (nasya) for nasal lubrication and protection, particularly during dry seasons or when spending extended periods in air-conditioned environments. Maintain regular practice of selected pranayama techniques, documenting effects on symptoms and functional capacity to identify optimal practices for individual physiology. During acute respiratory infections, combine modern symptomatic treatments with traditional remedies such as properly prepared kadha, understanding that complementary mechanisms may enhance overall effectiveness while reducing medication requirements. For chronic conditions, work with healthcare providers open to integrative approaches who can coordinate care across systems, ensuring interventions from different traditions do not interact adversely. Periodically reassess respiratory status through modern diagnostic methods, objectively evaluating whether integrated lung health protection strategies are achieving desired outcomes and adjusting protocols accordingly. This thoughtful integration honours both traditions while optimizing individual respiratory health.
9: Tobacco Cessation and Environmental Smoke Elimination

Comprehensive Approaches to Respiratory Toxin Elimination Through Lung Health Protection Strategies
Tobacco use remains the single most preventable cause of respiratory disease globally, yet its elimination from individual lives and community environments requires far more than simple willpower or awareness. The addictive potential of nicotine, delivered through smoking in ways optimized for rapid brain penetration and reinforcement, creates neurobiological changes that persist long after the decision to quit has been made. The behavioural rituals accompanying smoking become deeply ingrained habit patterns triggered by environmental cues, social situations, and emotional states that continue eliciting craving even after pharmacological dependence has been addressed. Beyond active smoking, second-hand and third-hand smoke exposure continues damaging respiratory health of non-smokers who live, work, or socialize in environments where others have smoked. The persistence of tobacco residues on surfaces, in dust, and adsorbed to fabrics means respiratory protection requires not only smoke-free policies but also remediation of contaminated environments. These complexities demand comprehensive lung health protection strategies addressing pharmacological, behavioural, and environmental dimensions of tobacco-related respiratory injury.
Advanced Understanding of Tobacco’s Respiratory Effects
The mechanisms through which tobacco damages respiratory tissues extend far beyond the carcinogenic effects dominating public discourse. Each cigarette exposes airways to over 7000 chemical compounds, hundreds of which demonstrate direct toxicity while dozens act as recognized carcinogens. The particulate phase of smoke paralyzes ciliary function within hours of exposure, temporarily disabling the mucociliary escalator that normally clears inhaled particles and pathogens from airways. This paralysis explains the characteristic smoker’s cough, an attempt to compensate manually for failed automatic clearance, while creating windows of vulnerability during which other inhaled agents cause enhanced injury. Chronic exposure induces mucous gland hyperplasia and goblet cell metaplasia, increasing mucus production while simultaneously impairing its clearance, creating the productive cough and recurrent infections characterizing chronic bronchitis. The inflammatory response to smoke constituents recruits neutrophils and macrophages that release proteolytic enzymes, gradually destroying alveolar walls in emphysema while stimulating fibroblast proliferation that narrows small airways in peribronchiolar fibrosis. Simultaneously, smoke components deplete antioxidant defences while activating cytochrome P450 enzymes that generate additional reactive species, overwhelming protective mechanisms and accelerating tissue aging throughout the respiratory tract. Understanding these mechanisms reveals why no level of tobacco exposure can be considered safe and why aggressive lung health protection strategies targeting elimination are essential.
Practical Pathways to Smoke-Free Living
For current tobacco users, develop structured cessation approaches recognizing the multifactorial nature of dependence and the need for sustained support. Consult healthcare providers about pharmacotherapy options including nicotine replacement therapy in various forms, bupropion, or varenicline, understanding that medication roughly doubles cessation success rates compared to willpower alone. Combine pharmacological support with behavioural interventions addressing smoking triggers and developing alternative responses to situations previously eliciting tobacco use. Access resources including national quitline services, community support groups, or digital applications providing structured cessation programmes and ongoing encouragement. Recognize that most successful quitters require multiple attempts before achieving permanent abstinence, treating each attempt as learning experience rather than failure. For non-smokers, establish and enforce smoke-free home and vehicle policies that protect all occupants from second-hand exposure, communicating these expectations clearly to visitors and family members. In public spaces, exercise right to clean air by moving away from smokers and advocating for stronger smoke-free policies in workplaces, restaurants, and public areas. When acquiring previously occupied homes or vehicles, consider professional cleaning to remove third-hand smoke residues embedded in fabrics, carpets, and ventilation systems. These comprehensive lung health protection strategies eliminate the most significant controllable respiratory risk factor while creating environments supporting sustained respiratory health.
10: Lifelong Respiratory Surveillance and Health Maintenance

Developing Personal Respiratory Health Systems Through Lung Health Protection Strategies
Respiratory health, like cardiovascular health or metabolic function, requires lifelong attention and systematic maintenance rather than episodic crisis intervention. The accumulation of environmental exposures, the natural aging process affecting lung tissue elasticity and respiratory muscle strength, and the potential for disease development at any life stage all demand ongoing surveillance capable of detecting changes early when intervention proves most effective. Building a personal respiratory health system means establishing routines for monitoring, maintaining professional relationships supporting timely intervention, and continuously updating knowledge as understanding evolves and new threats emerge. This systems approach transforms respiratory care from reactive problem-solving into proactive health optimization, shifting focus from treating established disease to maintaining optimal function throughout life. The investment required for such systems proves trivial compared to costs of disability, treatment, and lost quality of life when respiratory disease progresses undetected. These comprehensive lung health protection strategies represent the ultimate expression of personal responsibility for respiratory health.
Components of Effective Respiratory Surveillance Systems
Establish regular professional evaluation as foundation of respiratory surveillance, scheduling annual health maintenance visits specifically addressing respiratory status even in absence of symptoms. During these visits, review any respiratory symptoms experienced since previous evaluation, document changes in functional capacity or exercise tolerance, and perform objective testing including spirometry to detect changes before they become subjectively apparent. Maintain personal health records documenting these evaluations, creating longitudinal data revealing trends that single measurements might miss. Stay current with recommended vaccinations including annual influenza immunization and pneumococcal vaccination according to age and risk factor guidelines, recognizing that vaccine-preventable infections cause substantial respiratory morbidity and may precipitate chronic disease exacerbations. Understand family history implications for personal risk, recognizing that genetic factors influence susceptibility to asthma, COPD, and lung cancer, warranting enhanced surveillance when family history indicates increased risk. Remain informed about emerging respiratory threats including novel viruses, changing pollution patterns, or occupational hazards relevant to current work or living situations, adjusting lung health protection strategies as circumstances evolve.
Creating Sustainable Health-Maintenance Behaviours
Transform respiratory surveillance from occasional obligation into integrated life routine through behavioural design making healthy choices automatic rather than effortful. Link respiratory health activities to established habits, performing breathing exercises after morning hygiene routine or checking AQI while having morning tea, creating implementation intentions that fire automatically when triggering events occur. Share respiratory health goals with family members, enlisting social support and accountability while potentially improving health of entire household. Document progress and setbacks in simple journal or application, creating feedback revealing patterns and motivating continued effort. Celebrate milestones in respiratory health maintenance, whether completing year without respiratory infection, maintaining exercise capacity through seasonal challenges, or achieving smoking cessation anniversary, reinforcing behaviours through positive recognition. Remain flexible as circumstances change, adjusting lung health protection strategies when moving to new location, changing occupations, or entering different life stage requiring modified approaches. This systematic approach transforms respiratory health from abstract concern into concrete reality, empowering individuals to breathe freely and live fully throughout their natural lifespan.
Conclusion: Taking Control of Your Respiratory Destiny Through Consistent Application

As we reach the end of this comprehensive exploration of respiratory health in modern India, the most important message to carry forward is that you possess far more power to protect your lungs than you might have realized before reading this guide. The challenges are real and they are serious, with air pollution reducing life expectancy by years across our nation and lung diseases hiding silently in millions of undiagnosed individuals. However, the solutions are equally real and equally powerful when applied consistently over time. The ten strategies presented throughout this guide work together as an integrated system, each one reinforcing and amplifying the benefits of the others. When you invest in HEPA filtration for your home, you are not just buying an appliance, you are creating a sanctuary where your lungs can recover from daytime exposures and repair the microscopic damage that accumulates during outdoor activities. When you incorporate amla, turmeric, and ginger into your daily diet, you are not just following traditional wisdom, you are delivering concentrated antioxidants directly to the cells lining your airways, helping them neutralize the oxidative stress caused by inhaled pollutants before it can trigger inflammation or DNA damage. When you practice diaphragmatic breathing for ten minutes each day, you are not just relaxing, you are strengthening the primary muscle of respiration while improving ventilation to lung regions that typically remain underused, thereby enhancing overall gas exchange efficiency and building respiratory reserve that will serve you well as you age. The winter-specific precautions described in this guide acknowledge that seasonal variations demand seasonal responses, and by adjusting your exercise timing, mask usage, and indoor humidity management as temperatures drop, you can continue living actively while avoiding the peak dangers of cold-weather pollution inversions. Exercise itself emerges as a non-negotiable pillar of respiratory health, not merely for cardiovascular reasons but because physical activity stimulates angiogenesis in pulmonary capillaries, upregulates antioxidant enzymes throughout respiratory tissues, and maintains the strength of ventilatory muscles that would otherwise weaken with age and inactivity. The integration of traditional Indian healing practices with modern medical science offers the best of both worlds, allowing you to benefit from millennia of observational wisdom while also accessing precise diagnostic tools and evidence-based treatments when needed. Tobacco cessation deserves special emphasis as the single most impactful intervention anyone can make, whether by quitting active smoking or by establishing smoke-free environments that protect non-smoking family members from second-hand and third-hand exposure. The lifelong surveillance system described in our final strategy ensures that you do not become complacent, that you continue monitoring your respiratory status through regular check-ups and spirometry testing, catching any problems early when they remain most treatable. Perhaps most importantly, this guide has emphasized throughout that perfection is not required and that every positive step you take, no matter how small, contributes to better respiratory health. Installing one air purifier in the bedroom where you sleep provides eight hours of clean air daily, which alone reduces your total pollution exposure significantly. Adding one antioxidant-rich food to your daily diet increases your internal defence capacity. Learning one breathing technique gives you a tool you can use anytime, anywhere, to calm your nervous system and improve ventilation. These small steps accumulate over time, building a foundation of respiratory resilience that protects you not only from today’s pollution but also from the accumulated effects of years of exposure. The future of respiratory health in India depends partly on policy changes and technological advances that lie beyond individual control, but it depends equally on millions of individuals making the conscious decision to protect themselves and their families using the tools already available. You are now equipped with knowledge that places you among the most informed people in the country regarding respiratory protection. The next step is action, starting today, starting now, with whatever small change fits easily into your current routine. Your lungs will thank you with every breath you take, today, tomorrow, and for all the years to come.
Frequently Asked Questions About Lung Health Protection Strategies
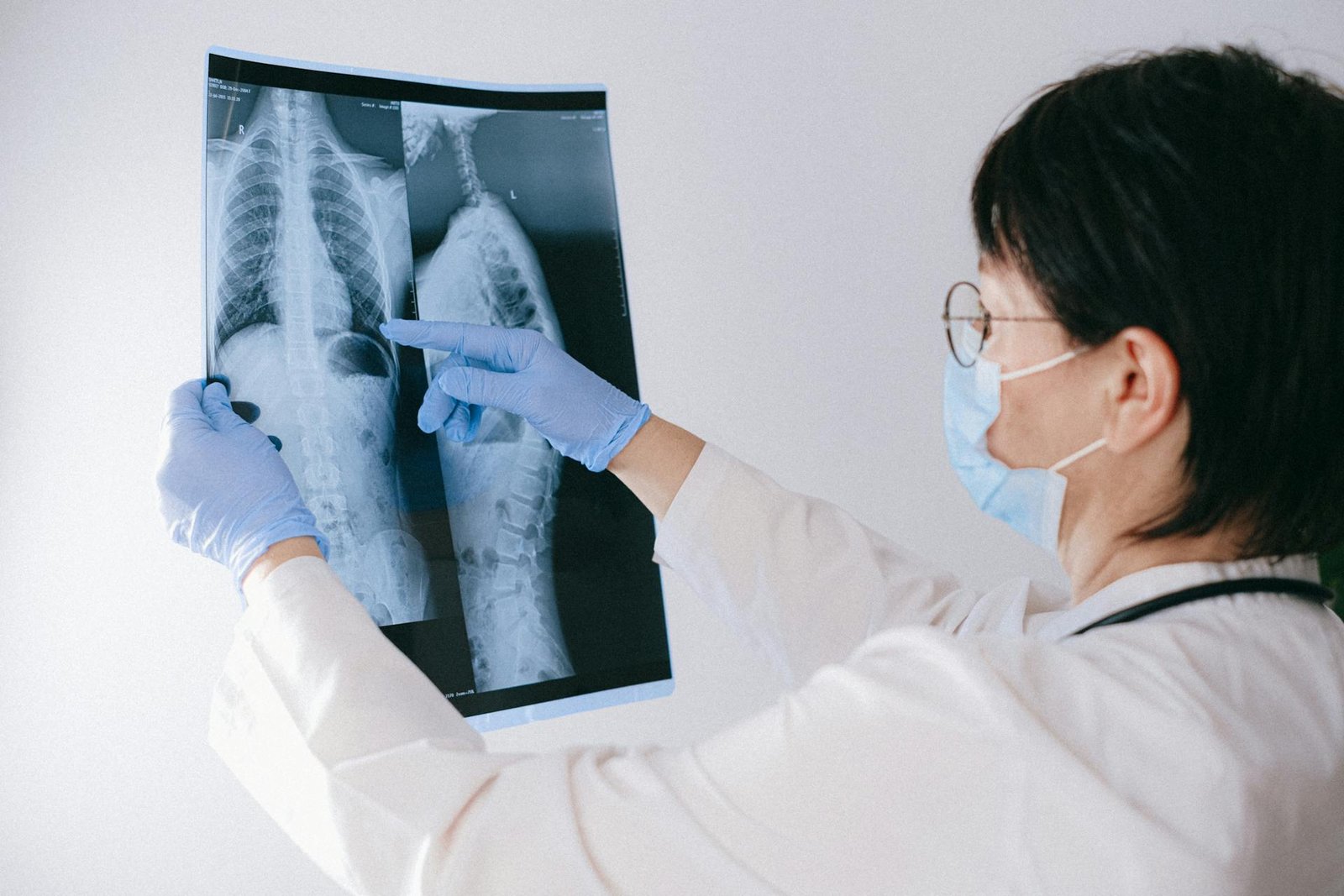
Question 1: What is the single most important thing I can do today to protect my lungs from Delhi’s terrible air pollution?
The most impactful immediate action you can take is to ensure your sleeping environment provides clean air throughout the night. Purchase a HEPA air purifier rated for your bedroom size and run it continuously while you sleep. This single intervention gives your lungs approximately eight hours of recovery time during which they are not fighting against inhaled pollutants, allowing natural repair mechanisms to address damage accumulated during daytime hours. During those eight hours, your respiratory tissues can restore depleted antioxidant reserves, clear out particles trapped in mucus, and reduce inflammation that would otherwise persist and worsen. If purchasing a purifier immediately proves difficult, create the cleanest possible sleeping space by wet-mopping floors, removing dust-collecting items, keeping windows tightly sealed, and placing a damp cloth over a box fan as a temporary filtration measure. This nightly clean air interval proves particularly crucial for children, whose developing lungs remain more vulnerable to pollution damage, and for elderly family members whose repair mechanisms operate less efficiently. The second most important immediate action involves checking the AQI before any outdoor activity and wearing an N95 mask whenever levels exceed 150, recognizing that visible smoke or haze indicates severe pollution but that invisible pollution often proves equally dangerous.
Question 2: How do I know if my cough is just a normal seasonal cough or something more serious requiring doctor attention?

Differentiating between benign seasonal cough and cough signalling underlying disease requires attention to duration, character, and associated symptoms that provide valuable diagnostic clues. Any cough persisting beyond three weeks warrants professional medical evaluation regardless of apparent severity, as acute infections typically resolve within this timeframe while persistent cough suggests ongoing pathology requiring investigation. The character of your cough matters significantly, with dry, tickling cough often indicating allergic irritation or early asthma, while productive cough bringing up yellow, green, or brown mucus suggests infection or chronic bronchitis requiring specific treatment. Pay close attention to associated symptoms including chest pain during deep breathing, unexplained fatigue disproportionate to activity level, unintentional weight loss, or fever that comes and goes without obvious explanation. Notice whether cough worsens at specific times, such as immediately after waking, during exercise, or when exposed to cold air or strong smells, as these patterns help distinguish different conditions. Perhaps most importantly, monitor for shortness of breath during activities that previously felt easy, such as climbing stairs, walking briskly, or carrying groceries, as declining exercise tolerance often indicates progressive lung disease long before resting symptoms appear. Any episode of coughing up blood, even if only a small streak, requires immediate medical attention as this symptom always indicates significant pathology needing urgent evaluation. Remember that India’s high rate of undetected lung disease means that assuming your symptoms represent nothing serious proves far more dangerous than seeking professional opinion that confirms your suspicion of benign condition.
Question 3: Can breathing exercises really help if I already have asthma or COPD diagnosed by my doctor?
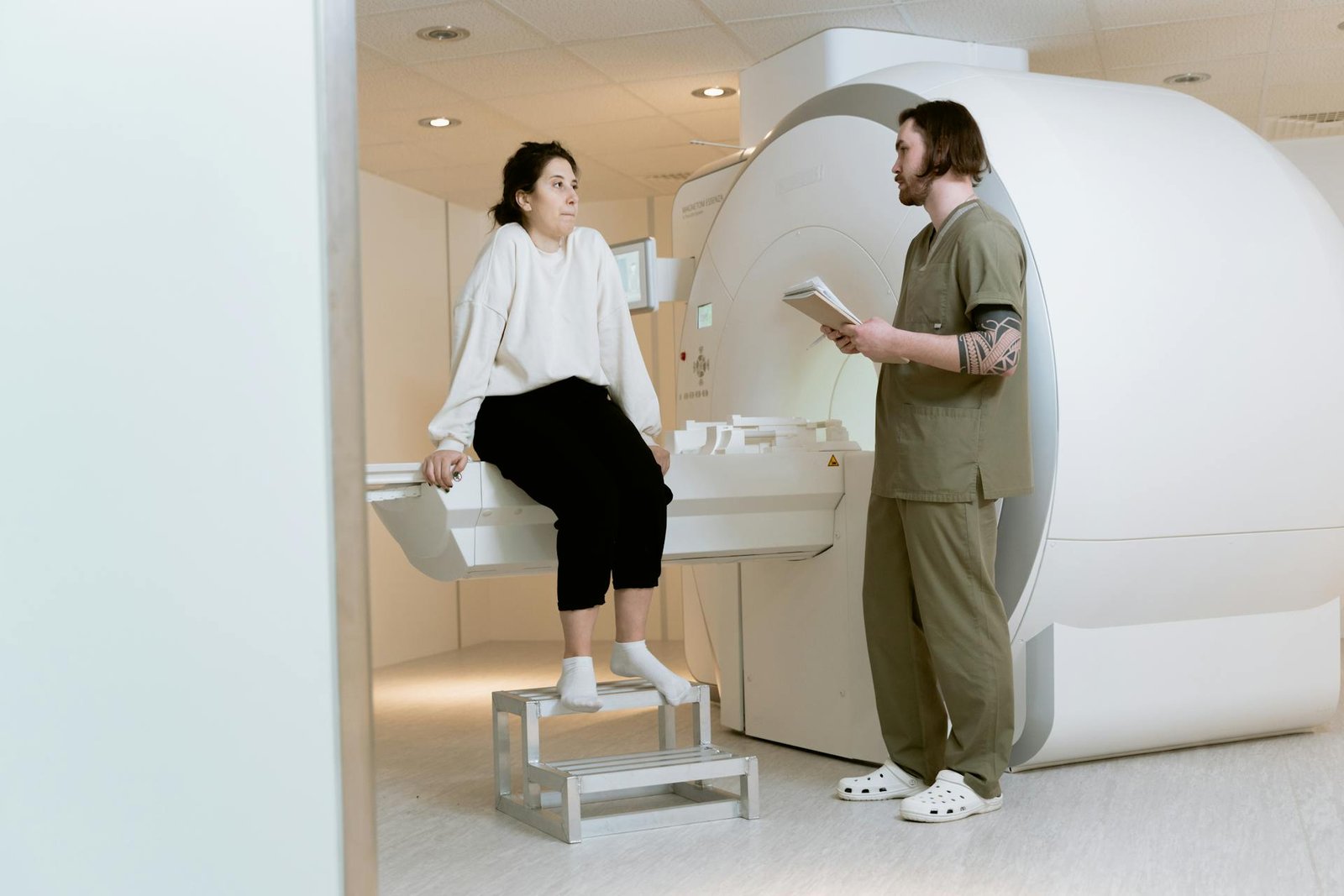
Breathing exercises provide clinically significant benefits for individuals with diagnosed asthma or COPD when properly performed and integrated with prescribed medical treatment rather than used as replacement for medication. Research studies demonstrate that regular practice of diaphragmatic breathing improves ventilation efficiency, reducing the work of breathing and decreasing the sensation of breathlessness that limits activity in chronic lung disease. Pursed-lip breathing, in particular, helps individuals with obstructive lung disease by generating back-pressure within airways during exhalation, preventing premature airway collapse and allowing more complete lung emptying before the next breath. This technique proves especially valuable during acute shortness of breath episodes, providing immediate symptom relief while waiting for medications to take effect. Pranayama techniques including Anulom Vilom have shown benefits for asthma patients in multiple clinical trials, with mechanisms including reduced airway inflammation, improved autonomic nervous system balance, and decreased sensitivity to bronchoconstricting triggers. However, you must never stop or reduce prescribed medications without consulting your doctor, as breathing exercises complement rather than replace pharmacological treatment. Begin breathing practice under guidance from respiratory therapist or trained yoga instructor who understands your specific condition and can ensure proper technique that maximizes benefit while avoiding any strain. Document your symptoms and medication use before starting breathing exercises and continue documentation afterward, creating objective record revealing whether techniques provide meaningful benefit for your individual case.
Question 4: How effective are indoor plants like snake plants and aloe vera at cleaning air in my home?

Indoor plants contribute modestly to air quality improvement but cannot substitute for mechanical filtration systems when addressing the severe pollution levels common in Indian cities. The famous NASA study demonstrating plant air-purifying capacity occurred in sealed laboratory chambers with conditions dramatically different from actual homes, and subsequent research shows that achieving meaningful air cleaning with plants alone would require approximately 10 to 100 plants per square metre of floor space, densities obviously impossible in normal living spaces. However, plants do provide real benefits including modest VOC absorption, humidity regulation that supports respiratory mucosal health, and psychological benefits that reduce stress, which indirectly benefits respiratory function through reduced inflammatory responses. Snake plants, spider plants, and aloe vera rank among the most effective common houseplants for air improvement, with snake plants offering the additional advantage of releasing oxygen at night rather than during daytime, making them particularly suitable for bedrooms. Position plants strategically in areas where you spend most time, ensure adequate light for their health, and maintain them properly because stressed or dying plants may release rather than absorb pollutants. The realistic approach combines HEPA filtration for primary air cleaning with selected plants providing supplementary benefits and aesthetic enjoyment that encourages spending more time indoors where air quality remains under your control.
Question 5: Is it safe for my children to play outside when the AQI shows moderate pollution levels around 150?

Children face heightened vulnerability to air pollution effects because their lungs continue developing through adolescence, they breathe more rapidly than adults, and they spend more time engaged in vigorous outdoor activity that increases both inhalation rate and depth. When AQI registers between 100 and 150, considered moderate on most scales, you should apply careful judgment based on your child’s individual health status and the specific activity planned. Healthy children without respiratory conditions can usually engage in moderate outdoor play during moderate AQI, but you should limit duration, avoid scheduling during peak pollution hours typically occurring early morning and evening, and choose locations away from traffic congestion. Children with asthma, allergies, or recurrent respiratory infections require stricter precautions even at moderate levels, with many pediatricians recommending indoor activities whenever AQI exceeds 100 for sensitive individuals. Watch for any symptoms during or after outdoor time, including coughing, wheezing, chest tightness, or unusual fatigue, and use these observations to adjust future decisions about acceptable activity levels. Teach children to breathe through nose rather than mouth during exercise when possible, as nasal passage filtration removes larger particles and warms inspired air before it reaches lungs. Ensure children wear appropriately fitted N95 masks during any outdoor time when AQI exceeds 150, recognizing that standard surgical or cloth masks provide inadequate protection against fine particulate matter. Most importantly, advocate at your children’s schools for indoor activity policies based on real-time AQI monitoring rather than fixed schedules, protecting all children regardless of individual sensitivity levels.
Question 6: How often should I replace the filters in my air purifier for optimal lung protection?
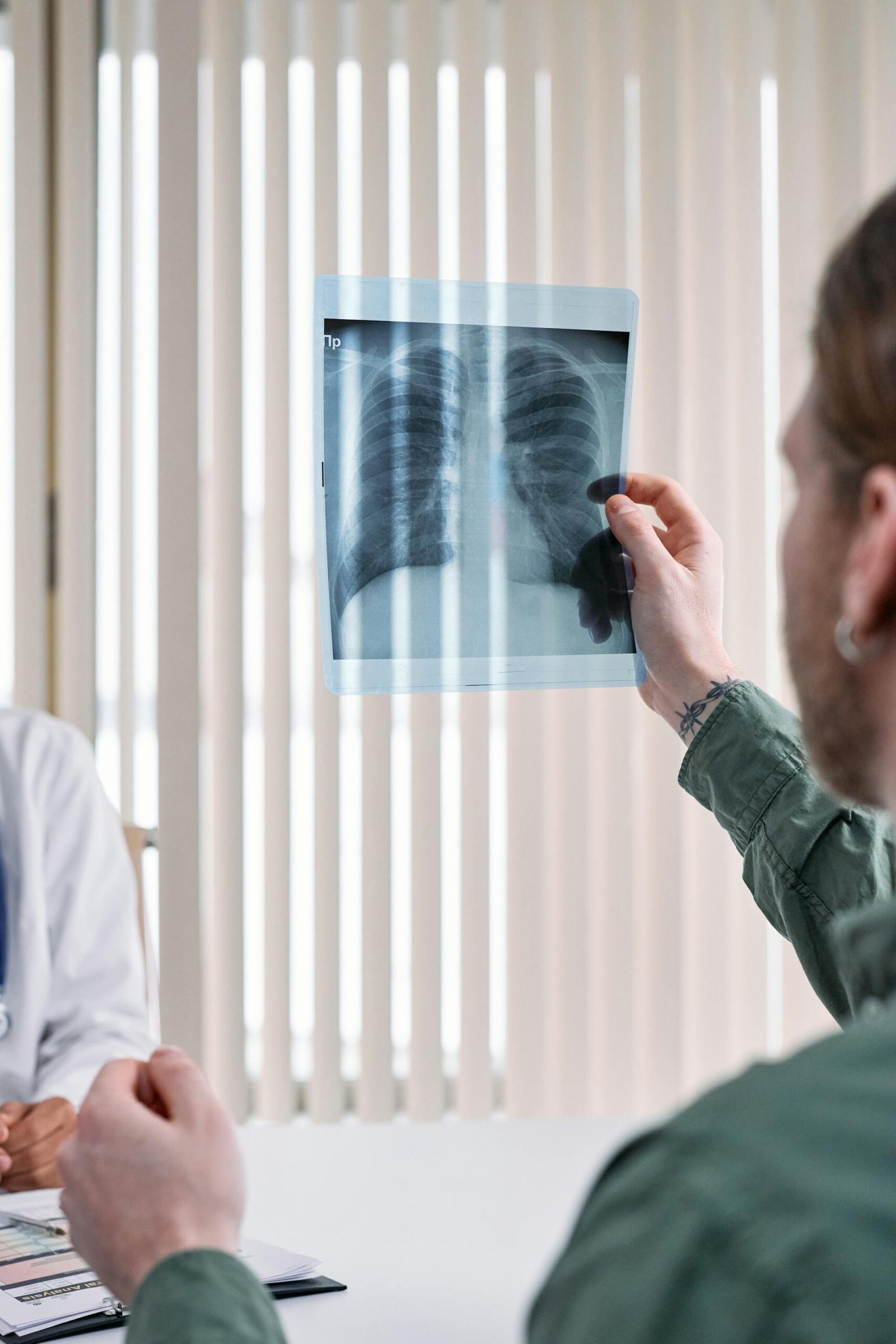
Filter replacement frequency depends on several variables including your purifier’s specifications, the pollution levels in your area, how continuously the unit operates, and the specific filter technology your device uses. Most manufacturers recommend replacing HEPA filters every six to twelve months under normal operating conditions, but in highly polluted Indian cities, filters may require replacement every three to six months to maintain optimal performance. Pre-filters, which capture larger particles before they reach the main HEPA filter, should be cleaned or replaced monthly, as clogged pre-filters force air through restricted pathways, reducing airflow and allowing particles to bypass filtration entirely. Many modern purifiers include filter replacement indicators that monitor actual filter loading rather than simply tracking calendar time, providing more accurate guidance about when replacement becomes necessary. You can supplement electronic indicators by monitoring airflow from your purifier, noting any significant reduction in output that suggests filter clogging, and by observing whether dust accumulates more rapidly on surfaces near the purifier, indicating reduced capture efficiency. Keep spare filters on hand to avoid operating periods with exhausted filtration, and purchase only genuine replacement filters matching your specific model, as counterfeit or incompatible filters may not seal properly, allowing unfiltered air to bypass filtration entirely. Record replacement dates on calendar and set reminders, making filter maintenance as routine as other household tasks rather than something you remember only when performance has already declined.
Question 7: Can traditional Indian remedies like kadha and haldi doodh really protect my lungs from pollution damage?

Traditional Indian remedies provide scientifically validated respiratory protection through multiple mechanisms that modern research continues to elucidate, making them valuable components of comprehensive lung health strategies rather than mere folk beliefs. Kadha, the traditional decoction combining herbs including tulsi, mulethi, black pepper, ginger, and other ingredients, delivers concentrated phytochemicals that demonstrate anti-inflammatory, antioxidant, antimicrobial, and immunomodulatory properties in laboratory studies. Tulsi contains compounds including eugenol and ocimumosides that reduce inflammatory signalling while enhancing natural killer cell activity that defends against respiratory pathogens. Mulethi provides glycyrrhizin with demonstrated antiviral activity and expectorant effects facilitating mucus clearance from airways. Black pepper’s piperine enhances absorption of other beneficial compounds while demonstrating its own anti-inflammatory effects. Haldi doodh delivers curcumin whose anti-inflammatory effects have been documented in hundreds of studies, though its poor natural bioavailability means combining with black pepper significantly enhances absorption. However, these remedies work best as preventive and supportive measures rather than acute treatments for established disease, and they complement rather than replace medical care when serious conditions develop. Prepare kadha properly by simmering rather than boiling to extract maximum compounds, consume it warm for best absorption, and maintain regular rather than occasional use for cumulative benefits. These traditional lung health protection strategies connect you with centuries of observational wisdom while delivering measurable physiological benefits that support respiratory health.
Question 8: What specific symptoms should make me rush to the hospital instead of waiting for a regular doctor appointment?

Certain respiratory symptoms indicate medical emergencies requiring immediate hospital evaluation rather than waiting for scheduled appointments, and recognizing these warning signs can literally save your life. Sudden, severe shortness of breath that prevents speaking full sentences or that occurs at rest demands emergency attention, as this may indicate pulmonary embolism, severe asthma attack, pneumothorax, or heart failure requiring immediate intervention. Chest pain that worsens with deep breathing or coughing, particularly if accompanied by shortness of breath, requires emergency evaluation to distinguish between pulmonary and cardiac causes. Coughing up blood, even in small amounts, always constitutes medical emergency requiring immediate hospital evaluation, as this symptom may indicate tuberculosis, pulmonary embolism, lung cancer, or severe infection needing urgent diagnosis and treatment. Blue discoloration of lips, fingertips, or skin indicates dangerously low blood oxygen levels requiring immediate supplemental oxygen and emergency care. High fever accompanied by severe cough, particularly if you feel confused or disoriented, suggests serious infection including pneumonia requiring hospital-level care. Sudden onset of sharp chest pain with shortness of breath after long travel or surgery raises concern for pulmonary embolism requiring immediate treatment. Any respiratory symptom that rapidly worsens over hours rather than days, or that follows exposure to known toxin or allergen, requires emergency evaluation. When in doubt, err on side of caution and seek emergency care, as the consequences of delaying treatment for serious respiratory conditions far outweigh inconvenience of unnecessary emergency visit that proves you were fine.
Question 9: How does smoking affect my lungs differently from air pollution, and is quitting still worth it after many years?

Smoking and air pollution damage lungs through overlapping but distinct mechanisms, with smoking delivering concentrated toxins directly to airways while pollution provides chronic low-level exposure, and quitting remains profoundly beneficial regardless of how long you have smoked or how much damage has already occurred. Cigarette smoke contains over 7000 chemical compounds, dozens of which are known carcinogens, delivered in highly concentrated form directly to lung tissue with each puff, creating intense local exposure that overwhelms defence mechanisms. The particulate matter in smoke paralyzes ciliary function within hours, disabling the natural cleaning system that normally removes inhaled particles and pathogens. Tar from smoke coats airways, delivering continuous chemical irritation while providing surface where carcinogens concentrate and bacteria adhere. Nicotine creates powerful addiction that maintains exposure despite known harms, distinguishing smoking from involuntary pollution exposure. However, pollution exposure continues 24 hours daily, creating cumulative oxidative burden that also drives disease, and the combination of smoking and pollution exposure multiplies risk beyond simple addition. When you quit smoking, your lungs begin healing within hours as carbon monoxide levels drop and oxygen delivery improves. Within weeks, ciliary function begins returning, improving clearance of mucus and particles. Within months to years, cough and shortness of breath decrease while lung function decline slows to rate of non-smokers. Even after lung cancer diagnosis, quitting improves treatment outcomes and reduces complications. The benefits of quitting at age 50, 60, or 70 remain substantial, adding years of life while improving quality of remaining years, making it never too late to gain from this most powerful of all lung health protection strategies.
Question 10: How can I protect my elderly parents living in small town or village where air purifiers and other resources may not be easily available?

Protecting elderly parents in resource-limited settings requires creative adaptation of core principles using locally available materials and practices, focusing on interventions that prove most impactful with minimal technological requirements. Start by addressing indoor air quality through practical modifications that anyone can implement regardless of location. Replace dry sweeping with wet mopping using simple cotton cloth and water, dramatically reducing dust resuspension without any special equipment. Create cross-ventilation during early morning hours when air quality typically improves, opening windows on opposite sides of home to flush out accumulated indoor pollutants. If cooking involves biomass fuels, the single most impactful intervention involves improving kitchen ventilation, whether through installing simple chimney, creating smoke outlet through wall, or cooking in separate structure when weather permits. Provide N95 masks and ensure parents understand when and how to wear them, emphasizing that visible smoke or dust indicates times requiring protection. Establish simple breathing exercise routine that parents can perform sitting comfortably, starting with just five minutes of deep breathing daily and gradually increasing as technique improves. Ensure regular medical check-ups including blood pressure and diabetes screening, as these conditions interact with respiratory health and prove particularly important when specialized lung testing unavailable. Teach recognition of warning signs requiring medical attention, writing them down clearly and posting where parents and caregivers can easily reference. Arrange telephone or video consultations with doctors when possible, using even basic mobile phones to connect with healthcare providers who can guide management without requiring travel. Coordinate with local relatives, neighbours, or community health workers who can check on parents regularly and help implement protective measures. These adapted lung health protection strategies prove that meaningful respiratory protection remains possible even without expensive technology, relying instead on knowledge, attention, and consistent application of basic principles that work anywhere.



1 thought on “Ultimate Lung Health Guide for Americans 2026”